Contraceptive is essential to family planning, but portrayed as something quite taboo in some countries. This is due to some cultures consider it to be morally, religiously, or politically undesirable, thus the access for it gets limited or discouraged. One of the popular and thought to be effective kind of contraceptive is the Intra-Uterine Device (IUD).
Despite it being said as an effective contraception, there are a lot of concern regarding IUD that seem to create hesitation. For example, there’s information that made some believe that IUD may cause fibroids, among other health risk and side effects. To avoid confusion and false pretences, let’s take a look into the facts about IUD.
What are They Saying About IUD?
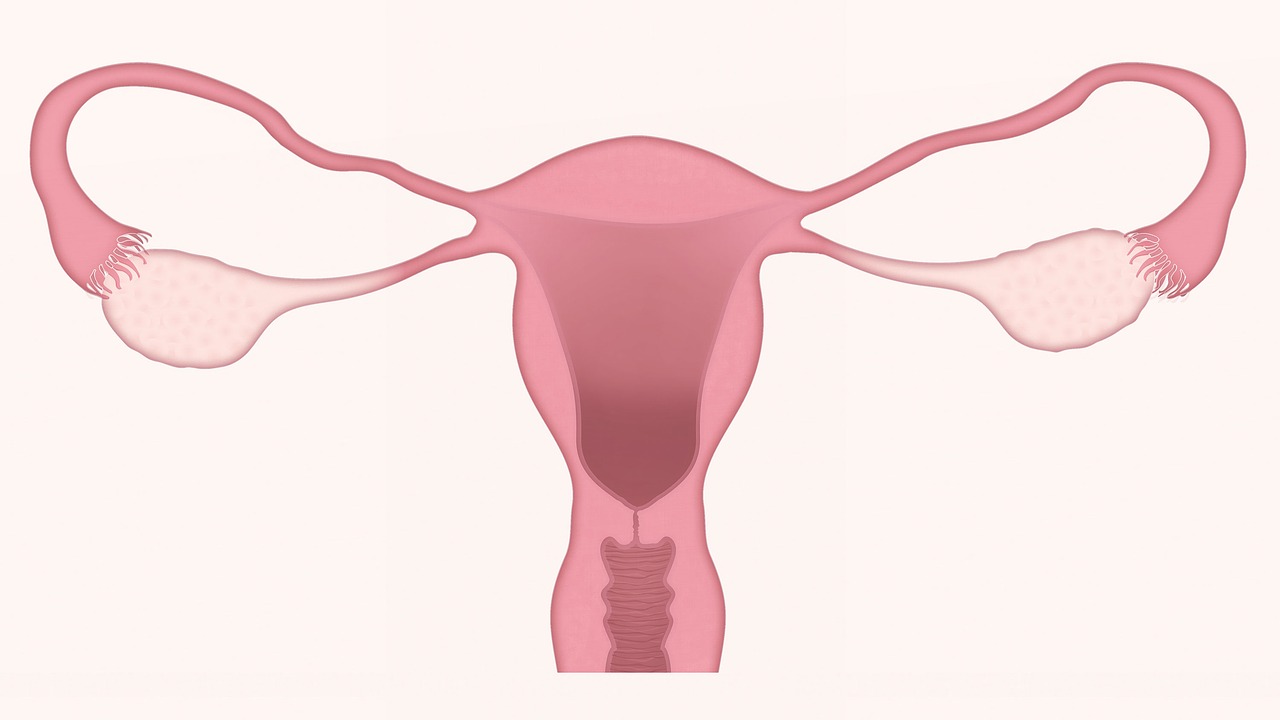
An intrauterine device (IUD) or coil, is a small, often T-shaped birth control device that is inserted into a woman's uterus to prevent pregnancy. Among birth control methods, IUDs, along with contraceptive implants, result in the greatest satisfaction among users. However, some women hesitate to use IUD because they question the safety of the contraception. Here are some of the myths that most couples believe about IUD…
Myth #
Myth #
Myth #
Fact : It might make you more relaxed about unintended pregnancies and enjoy sex even more!
Myth #4 : IUD prevents pregnancy by causing abortions.
Fact : IUDs do not work by causing abortions
Myth #5 : IUD is not effective in preventing pregnancy or that the IUD loses its contraceptive effect after only a few years from the time of insertion.
Fact : IUDs are the more than 99% effective!
Understanding the Health Risk & Side Effects of IUD
Some women do not want to use the IUD because they incorrectly believe that IUD causes side effects or health risks such as cancer, sexually transmitted infections, or birth defects.
The IUD never travels to the heart, brain, or any other part of the body outside the abdomen. The IUD normally stays within the uterus like a seed within a shell. Rarely, the IUD may come through (perforate) the wall of the uterus into the abdominal cavity. Proper insertion technique can help prevent many problems, such as infection, expulsion, and perforation.
IUDs do not cause cancer in otherwise healthy women, but confirmed or suspected cancer of the genital tract is a contraindication to IUD use, because the increased risk of infection, perforation, and bleeding at insertion may make the condition worse. For the levonorgestrel-releasing IUD, breast cancer is also a contraindication.
IUDs do not increase the risk of contracting STIs, including HIV. However, usually, women who have a very high risk of exposure to gonorrhea or chlamydia should not have an IUD inserted. In special circumstances, when other, more appropriate methods are not available or acceptable to her, a qualified provider who can carefully assess a specific woman’s risk may decide that she can use an IUD.
IUD use neither causes multiple pregnancies after removal nor increases the risk of birth defects, whether the pregnancy occurs with the IUD in place or after removal. There is a higher risk of preterm delivery or miscarriage, including infected (septic) miscarriage during the first or second trimester, which can be life-threatening. Early removal of the IUD reduces these risks, although the removal procedure itself involves a small risk of miscarriage. There is no evidence of increased risk of fetal malformations, however.